
Part II of Bipolar II Disorder: Misunderstood and Misdiagnosed
“Hypomania is mania with a tether, and, while it might avert some of the financial and interpersonal disasters that unchecked mania may engender, it can still feel like a runaway train.” New York Times, The Problem With How We Treat Bipolar Disorder by Linda Logan
Imagine what it feels like to be constantly living life either chasing a runaway train (bipolar hypomania) or trying to find the escape from the blackest caves of the mind (bipolar depression). It would be difficult doing much more than having to manage one’s mood and energy level. But, this is what Bipolar II people do. Fifty-four percent of the time they have symptoms of the disorder. They are taken up most days with trying to manage their ever-changing biology that is easily thrown off by working too hard, stressful events, illness, diet and physical activity level.
Many of us either have family or friends who have the disorder or may have the disorder ourselves. Today’s post answers the questions that most us have about this very challenging mental health condition. What causes bipolar disorder? Why does it run in families? What makes the brain chemistry of bipolar persons so vulnerable to stress? Can Bipolar II disorder be treated or cured altogether? Do bipolar persons have a chance to lead fulfilling and productive lives?
It’s In the Genes
What causes Bipolar Disorder and why does it run in families?
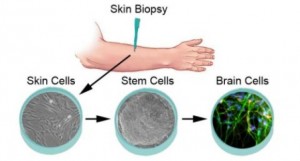 Bipolar disorder starts at the level of a gene. A whole symphony of genes that are coded for the disorder produce stem cells (the most basic of body cells) that differ from persons without the disease (Drugs for Bipolar Disorder Normalizes Gene Function). Stem cells are able to develop into blood, skin, and nerve cells that form the structure of our minds and bodies.
Bipolar disorder starts at the level of a gene. A whole symphony of genes that are coded for the disorder produce stem cells (the most basic of body cells) that differ from persons without the disease (Drugs for Bipolar Disorder Normalizes Gene Function). Stem cells are able to develop into blood, skin, and nerve cells that form the structure of our minds and bodies.
What makes bipolar persons so vulnerable to stress?
The brain chemistry of bipolar persons differs from people without the disorder. Recent studies show that the stem cells arising from genes coded for bipolar disorder multiply and develop into a highly distinctive and sensitive network of brain nerve cells. During brain activity, these nerve cells are positioned toward creating the biological upward and downward swings of mood, thinking, energy level and behavior that is seen in Bipolar Disorder I and II (First Stem Cell Study of BPD Yields Promising Results; Susceptibility factor in for Bipolar Disorder Identified). These nerve cells are highly sensitive to changes coming from inside (e.g., illness, allergies reactions, shifts in hormones, diet and exercise) or outside the person (e.g., job and relationship pressures and conflict, environmental changes of season, or threats to one’s security). This is why bipolar persons can’t take too much stress. As stressors build over time, the brain of bipolar people is more apt to shift to a depressed, manic, or hypomanic state (Happiness and Sad Brain Circuits Role in Bipolar Disorder). What is more, prolonged stress or trauma can sensitize the bipolar brain to the point where now very little internal or external stimulation is needed to shift the brain’s circuits to depression, mania or hypomania (known as the kindling effect).
Can Bipolar Disorder I and II be treated? Can people with the disorder live productive and fulfilling lives?
Bipolar Disorder I and II can be treated and well-managed but not cured. It is a high maintenance condition that leaves little to no budge room when it comes to self-care. A person can’t wish the sensitivities of the disorder away or ignore them without risking worsening symptoms and the chance of leading a productive and satisfying life.
Today, there is a lot more known about the disorder that has led to many new treatments. Many of the treatment recommendations mentioned below apply to both Bipolar I and II Disorder, other than the mood stabilizing medication Lithium that is the first line of treatment for mania in Bipolar I Disorder.
Bipolar persons thrive when they learn how to live a more balanced lifestyle that is gentler and kinder on their brain chemistry and bodies. They need to consider the physical, emotional, sexual and spiritual aspects of their lives that are affected by the disorder and learn to compensate for them through proper treatment and sound habit.
As you review the following recommendations remember that there can be a lot of differences between Bipolar II persons in terms of tolerance of stress, ego strength, coping resilience, patterns of mood swings, and degree of symptoms that has to do with co-existing personality disorders, such as Borderline Personality Disorder, traumatizing life events, alcohol or substance abuse, and quality of self-care habits.
A Gentler, Kinder Lifestyle
1. Medication: The Backbone of Bipolar Treatment: A number of medications treat Bipolar II Disorder. A mood stabilizer is often the first line of medication treatment, to lower the point at which the brain responds to internal and external change by a shift of mood. Anticonvulsants are typically used in Bipolar II disorder to stabilize mood rather than Lithium. The most popular anticonvulsant for Bipolar II treatment is Lamictal, approved by the food and drug administration for treatment of hypomania. Lamictal is particularly effective at preventing relapse of depression that is an important benefit for Bipolar II depression that is chronic if untreated.
Other anticonvulsants used to treat the disorder include Depakote (levels out moods and works more quickly than lithium therapy), Tegretol and Trileptal. Only in extreme hypomanic states in which there is a lot of destructive, acting out behavior is Lithium used, but this is after there has been a trial of Lamictal and the other anticonvulsant mood stabilizers. Lithium is a powerful salt that alters the balance of minerals inside and outside nerve cells. At specific levels, lithium prevents nerve cells from firing too fast or too slow that stabilize the mind and consequently mood, energy and activity level.
Benzodiazepines (tranquilizers) may be added (Ativan, Xanax, and Valium) for the short-term control of severe symptoms common with hypomania, such as agitation or insomnia.
Antidepressants are often the second line of treatment, although it is common that people with the disorder are already on antidepressant medication for depression that has been misdiagnosed as a unipolar, major depression. This is only a problem if the antidepressant is of the type that can actually stimulate hypomania. Among the antidepressants, the FDA has only approved Seroquel and Seroquel XR for the treatment of bipolar II depression. Other antidepressants sometimes prescribed to treat depression include Paxil, Prozac, and Zoloft. But, these medications are less effective because they tend to cause or worsen symptoms of hypomania in Bipolar II Disorder, especially Zoloft.
Recent drug studies show that the newer antipsychotic medications appear to nudge genes involved in bipolar illness into a pattern of expression that resembles normal brain chemistry (Drugs for Bipolar Disorder Normalizes Gene Function: First Stem Cell Study on Bipolar Illness Yields Promising Results). It is thus popular now to include these medications in the treatment of Bipolar II disorder, even though a person’s hypomanic symptoms do not include psychosis or may not interfere with functioning. Antipsychotic medications include Latuda, Abilify, Seroquel, Risperdal, and Geocon.
2. Psychotherapy: Psychotherapy is a very important aspect of Bipolar II treatment. It’s important to learn how to cope with the effects of the disorder on one’s life, to teach lifestyle skills and habits that help to manage the symptoms of the disorder and to cope with suicidal tendencies. Studies show that people with Bipolar II Disorder who are educated in the disorder, understand its signs and symptoms, and develop a lifestyle that helps to manage the disorder are more mentally and emotionally stable than persons being treated with medication alone (Psychoeducation for bipolar II disorder: An exploratory, 5-year outcome sub analysis).
Cognitive-behavioral therapy (CBT) and Dialectical Behavior Therapy are psychotherapies most often used to treat Bipolar II disorder. These psychoeducational and skill-based therapies educate about the disorder and its treatments and teach skills to manage symptoms of the disorder and to prevent their relapse. They also teach coping techniques to manage stress level, alter thought patterns that lead to depressed or hypomanic mood, and regulate emotions. Learning how to regulate emotions is essential to any bipolar treatment program. Many studies show that bipolar people benefit from mindfulness based therapies that teach them how to stay aware of thoughts and feelings that tend to shift their moods, if indulged (Mindfulness-Based Cognitive therapy helps bipolar people; (Mindfulness Therapy Helps Relapse in Depression; Mindfulness Based Cognitive Therapy Improves Frontal Control in Bipolar Disorder).
Psychotherapy is also helpful in treating mental health conditions that may accompany Bipolar II disorder (e.g., acute conditions of alcohol or substance abuse, anxiety, Post Traumatic Stress, Social Phobia, or Attention Deficit disorders or Borderline Personality Disorder).
3. Diet: Diet can positively or negatively affect the brain’s functioning. Food is really a medicine, after all. It provides us with necessary nutrients to repair and build the body and affects the concentration of minerals in the body’s fluids and blood gases that can activate or inhibit the activity level of the brain and nervous system. As you can imagine, diet can increase or decrease bipolar symptoms that has implications for functioning and amount of medication.
Studies show that a diet that increases omega 3 fatty acids, reduces calcium overload and also lowers glutamatergic activity (Bipolar Disorder and Glutamate) in the brain are very helpful to controlling the biological swings of bipolar disorder, I and II and preventing a relapse of symptoms.
A Ketogenic diet (lower in carbohydrates and higher in fat) is recommended to reduce an overload of calcium that increases the rate of nerve firing and causing biological swings in bipolar persons. Lowering carbohydrates promotes a state of ketosis in the body that decreases the amount of sodium floating outside body cells. This shifts the rate at which the nerves fire and is helpful to stabilizing mood in bipolar disorder. Anticonvulsants essentially do the same thing as ketosis; they reduce extracellular levels of sodium.
Studies also show a relationship between the excitatory nerve transmitter glutamate and bipolar mania and hypomania (Rapid Enhancement of Glutamatergic Neurotransmitter in Bipolar Disorder). Glutamate lowers the inhibitory neurotransmitter called GABA(gamma aminobutyric acid) that can trigger a hypomanic and manic episode. The anticonvulsants and anti-anxiety medications used to stabilize brain activity in bipolar disorder reduces acute symptoms of hypomania and mania because they lower glutamate in the brain that reestablishes normal levels of GABA.
Lowering foods high in glutamate can help to stabilize mood, energy and activity levels. Foods to avoid include include grains (wheat, barley and oats are the highest); dairy products (all cheeses, especially aged cheese and casein is 20% glutamic by composition); beans (soy, pinto, lima, black, navy and lentils); seeds (sunflower and pumpkin), peanuts (including cashews, pistachios and almonds); prepared foods (70% of them, like soup contain monosodium glutamate), and meats (all meats are naturally high in glutamate—lamb is the lowest, while rabbit and turkey the highest). Any food that has monosodium glutamate or has been aged, matured, cured, preserved or fermented should be altogether avoided.
Bipolar persons are at higher risk for hyperthyroidism, migraine headaches, heart disease, diabetes, obesity, and other physical illnesses because of chemical imbalances but also may result from some of the medication treatments of bipolar disorder (National Institute of Mental Health: Bipolar Disorder). It is thus very important to establish a diet that may reduce the need for large amounts of medication and lower the risk of disease.
4. Exercise: Improving overall health through exercise is an important part of bipolar lifestyle management (Exercise Benefits Bipolar Disorder). It can help to manage side effects from medication such as weight gain, increase feel good chemicals like endorphins and serotonin, calm anxiety and improve sleep. Studies show that yoga helps to reduce stress overload, relax the mind and body, and improve the overall health and self-esteem of bipolar persons.
A holistic treatment approach is essential to treating bipolar disorder. The high risk of suicide typical in Bipolar Disorder decreases when bipolar persons are medically treated and leading a lifestyle that reduces symptoms and permits them to amply work, love and play. The only thing that may stand in the way of a productive and fulfilling life for Bipolar II persons is their dedication to maintaining a lifestyle that treats their disorder.
I hope you liked my post today. If so, please let me know by selecting the Like icon that follows. You can also Tweet or Google+1 today’s post to let your friends know about it. Take good care of yourself. Warm regards to all, Deborah.
Links to Book Resources for Bipolar Disorder:
Bipolar II Workbook, New Harbinger Publications
Dialectical Therapy Workbook: Amazon.com
The Tao of Bipolar Disorder: Using Meditation and Mindfulness to Find Balance: Amazon.com
Bipolar Disorder: A Guide for the Newly Diagnosed: Amazon.com
Bipolar Disorder Group on Google (Founder–and my friend- Vijay Nallawalla)







Excellent and informative article..I was diagnosed with BIPOLAR 2, few years ago. Thank you.
Hello Karen, I’m sorry for the delay in getting back to you. I’m so glad that you found this article helpful. Well, one thing is you are in very good company with the disorder as you know. The many new insights into the origins of the disorder that have led to better treatments are so promising to any person who has Bipolar II disorder. Glad to say hello to you Karen. Take good care. Deborah.
I wish I understood all of what you said. Just amazing!
Oh thank you so much Rita. It’s good to say hello to you here. Warmly Deborah (And the gang too!).
really great post, id like to ad some info if thats ok with everyone.
http://dinomoz.com/thread-post-traumatic-stress-disorder-ptsd-test-symptoms-and-help
Hi David, by all means add in a comment. Oh, I see you put a link in your comment. Thanks David. Warm regards Deborah.
Such a wonderful article. Thank you for addressing Bipolar 2 and for the excellent information. I was diagnosed with Bipolar 2 in the early 1980s at age 36. After a full decade of continuous depression, 12 medication trials, and three hospitalizations; Prozac hit the market, and that finally did it for me. Night and day difference! You are so right that Bipolar is lifelong, and I do have to stay on top of it at all times. I have been doing research again on bipolar as I have had a debilitating relapse in depression over the last 2-3 years. Unfortunately, my current psychiatrist does not seem to know what to do with me, and so I have suffered much much longer than I should have to. Nice enough man, but I finally had to fire him yesterday. I will be seeing someone new, and I won’t give up until I get to a better place again. After what I’ve been through, I know that’s possible.
Hello Miriam, You are very welcome. I know that this disorder is very difficult to diagnose and often missed until a person is past their 30’s or 40’s. The lifelong depression that rarely a person knows unless experienced first hand is so burdensome. thank goodness now that our field really understands it and there are new treatments.
Oh, I’m sorry to hear about the ending of relationship with your psychiatrist. You know sometimes after going to someone a long time a new perspective helps. Glad to see you will be seeing someone else. As you most likely know Miriam, diet is very important to help you maintain, minimize your symptoms. So please check into this.
Warm regards to you, Deborah
This article tells you to stop eating food. What’s left when you cut out these out, just fish and vegetables?
Foods to avoid include include grains (wheat, barley and oats are the highest); dairy products (all cheeses, especially aged cheese and casein is 20% glutamic by composition); beans (soy, pinto, lima, black, navy and lentils); seeds (sunflower and pumpkin), peanuts (including cashews, pistachios and almonds); prepared foods (70% of them, like soup contain monosodium glutamate), and meats (all meats are naturally high in glutamate—lamb is the lowest, while rabbit and turkey the highest).